Pancreatic Cancer
Pancreatic Cancer
“God put the pancreas in the back because he did not want surgeons messing with it.”
Theodor Billroth; 1829- 1894
What is Pancreatic Cancer?
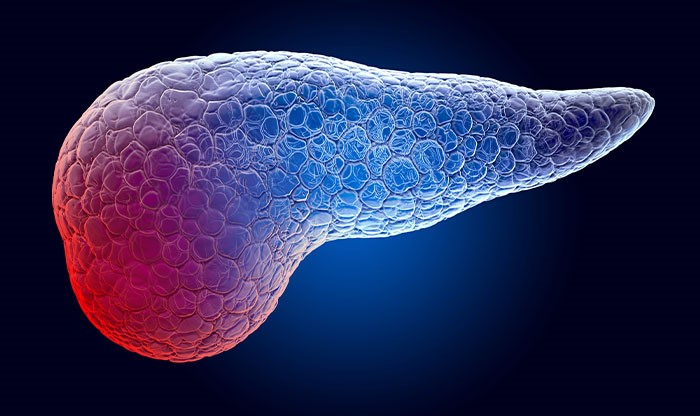
Pancreatic cancer begins in the pancreas, an organ located behind the lower part of your stomach. The pancreas has two main functions: it secretes enzymes that aid digestion and produces hormones that help regulate your blood sugar.
Various masses can form in the pancreas, including tumors made up of cancerous and non-cancerous cells. Not all masses found in the pancreas have to be cancerous. The most common type of pancreatic cancer starts in the cells that line the ducts carrying digestive enzymes away from the pancreas (pancreatic ductal adenocarcinoma).
Pancreatic cancer is most treatable at its earliest stage, but it is rarely detected at this stage. This is because it usually does not cause symptoms until it spreads to other organs.
Treatment options for pancreatic cancer are chosen based on the extent of the cancer and its location in the pancreas. Options may include surgery, chemotherapy, radiation therapy, or a combination of these.
What are the causes of pancreatic cancer?
The exact cause of pancreatic cancer is not known, but several risk factors have been identified that may increase the likelihood of developing the disease:
- Smoking: Tobacco use is a significant risk factor for pancreatic cancer.
- Age: The risk increases with age, particularly after the age of 50.
- Family history: A family history of pancreatic cancer may increase risk.
- Genetic mutations: Certain inherited genetic mutations can raise the likelihood of developing pancreatic cancer.
- Chronic pancreatitis: Long-term inflammation of the pancreas may contribute to the development of cancer.
- Diabetes: There is a link between diabetes and pancreatic cancer, particularly new-onset diabetes.
- Obesity: Being overweight or obese is associated with an increased risk of pancreatic cancer.
- Diet: A diet high in red and processed meats and low in fruits and vegetables may be linked to a higher risk
“Remember; scientific studies have proven that pancreatic cancer surgery tends to cause fewer complications when performed by highly experienced surgeons at centers that perform most of these surgeries. Don’t hesitate to ask your surgeon and hospital about their experience with pancreatic cancer surgery. If you have any doubts, seek a second opinion. Just don’t waste time.”
When Should I See a Doctor?
If you experience unexplained symptoms that worry you, consult your doctor. However, remember that the symptoms mentioned above are not specific to pancreatic cancer.
Why Do I Get Pancreatic Cancer?
The exact cause of pancreatic cancer is unclear. Smoking and having certain hereditary gene mutations are established risk factors.
Where Is My Pancreas? What Does It Do?
Your pancreas is located behind the lower part of your stomach, close to your back. It is about 15 cm long and is approximately 3 fingers below the end of your ribs. It has two main functions: the first is to regulate your blood sugar, and the second is to digest the food we eat.
How Does Pancreatic Cancer Develop?
Like many types of cancer, pancreatic cancer occurs when the cells in your pancreas develop changes (mutations) in their DNA. A cell’s DNA contains instructions that tell the cell what it should do. These mutations tell the cells to grow uncontrollably and continue living even after normal cells have died. The accumulating cells can form a tumor. If left untreated, pancreatic cancer cells can spread to nearby organs, blood vessels, and distant parts of the body. Spread is easier in pancreatic cancer because the pancreas has a rich blood supply due to its dual role in hormone production and digestion, allowing it to spread through blood and lymph nodes.
Most pancreatic cancers begin in the cells that line the pancreatic ducts. This type of cancer is called pancreatic adenocarcinoma or pancreatic exocrine cancer. Less commonly, cancer may form in the hormone-producing cells or the neuroendocrine cells of the pancreas. These cancers are called pancreatic neuroendocrine tumors, islet cell tumors, or pancreatic endocrine cancer.
What Are the Risk Factors?
Factors that can increase your risk of pancreatic cancer include:
- Smoking
- Diabetes (it is debated whether it is a cause or a result)
- Chronic inflammation of the pancreas (Chronic Pancreatitis)
- A family history of genetic syndromes that can increase cancer risk, including BRCA2 gene mutation, Lynch syndrome, and familial atypical mole-malignant melanoma (FAMMM) syndrome
- A family history of pancreatic cancer
- Obesity
- Aging, as most people are diagnosed after the age of 65
Important Note: A large study involving a significant number of patients showed that the combination of smoking, long-standing diabetes, and poor diet further increases the risk of pancreatic cancer beyond the risk posed by any of these factors individually.

What Are the Complications?
Weight loss: Weight loss can occur as cancer consumes the body’s energy. Nausea and vomiting caused by cancer treatments or a tumor pressing on your stomach can make eating difficult, leading to weight loss. Additionally, your body may struggle to process nutrients from food if your pancreas is not producing enough digestive enzymes.
Jaundice: Pancreatic cancer that blocks the bile duct in the liver can cause jaundice. Cancers located at the head of the pancreas can also block the bile duct. Symptoms include yellowing of the skin and eyes, dark urine, and pale stools (the color of putty, as described in the past). Your doctor may recommend placing a plastic or metal tube (stent) to keep the bile duct open. This can be done through a procedure called endoscopic retrograde cholangiopancreatography (ERCP). During ERCP, an endoscope is passed through your throat, stomach, and upper small intestine. A hollow tube (catheter) is then passed through the endoscope to inject dye into the pancreatic and bile ducts, which are imaged. If you’re scheduled for surgery early on, a catheter may be placed through percutaneous transhepatic cholangiography (PTC catheter) instead of ERCP. The choice between these methods depends on whether or when you’ll receive chemotherapy or surgery, and your surgeon will make this decision. If the tumor is too advanced for surgery and neither method is beneficial, your surgeon may recommend a surgery (hepaticojejunostomy) to connect the bile duct to the small intestine.
Pain: A growing tumor can press on nerves in your abdomen, causing pain, especially if it radiates to the back. Pain medications can help you feel more comfortable. Treatments such as radiation and chemotherapy can help slow tumor growth and provide some pain relief. However, back pain is not a favorable symptom for us clinicians. In severe cases, your doctor may suggest a procedure to inject alcohol into the nerves that control pain in your abdomen (celiac plexus block). This procedure blocks the nerves from sending pain signals to your brain.
Bowel obstruction: Pancreatic cancer that grows or presses on the first part of the small intestine (duodenum) can block the flow of digested food from your stomach to your intestines. Your doctor may suggest placing a tube (stent) in your small intestine to keep it open, or, if the tumor is too advanced for surgery, they may recommend a surgery to connect your stomach and intestines (gastrojejunostomy).
What Is Needed for Diagnosis? (What Tests Will My Doctor Order?)
Computed Tomography (CT) and/or Magnetic Resonance Imaging (MRI), Positron Emission Tomography (PET): These are imaging tests that create pictures of your internal organs. These tests help visualize your internal organs, including the pancreas. Based on these images, your doctor will inform you whether you are eligible for surgery and whether oncology treatment should occur before or after surgery. If there is tumor spread, the doctor will have an idea and will evaluate the conditions for surgery. Contrast agents are used in these imaging tests and are important for determining relationships with blood vessels.
Endoscopic Ultrasound (EUS): If your doctor does not reach a clear conclusion with the imaging tests described above or wants to be sure, they may request an EUS. It provides additional information and can be diagnostic in experienced hands. A biopsy is not necessarily required during the procedure. In fact, if there is a clear tumor image, a biopsy is not recommended.
Biopsy: To address a question I sometimes encounter from my patients: Will you operate without a biopsy diagnosis? If there is no doubt about the mass and no concern about chronic pancreatitis, then YES. This is because 10% of solid masses in the pancreas would not require surgery, but 90% are the kind where you’ll be glad you had surgery. To reiterate, a biopsy is not always necessary. Another example: If a biopsy comes back clean despite the presence of a tumor, the pancreas is not an organ where we can simply say you’re fine.
Blood Tests: Your doctor may test your blood for specific proteins (tumor markers) shed by pancreatic cancer cells. One tumor marker test used for pancreatic cancer is called CA19-9. It can help understand how well the cancer is responding to treatment. However, the test is not always reliable because CA19-9 levels do not rise in all people with pancreatic cancer, making it less useful. Blood tests are often necessary to check whether the mass is pressing on the bile duct, if it has affected the liver, caused an infection, or for surgical preparation. They are essential.
Staging: Your doctor will use a staging system to determine whether surgery is an option (whether your tumor is advanced) and whether preoperative chemotherapy is needed to shrink the tumor before surgery. Remember, this decision should not be made individually but should be determined in multidisciplinary (involving multiple specialties) meetings.
What Surgeries Are Performed on People with Pancreatic Cancer?
The pancreas can be divided into two sections: the body-tail and the head, according to the neck. If your tumor is in the head of the pancreas, you will undergo a surgery called the Whipple procedure (pancreaticoduodenectomy). The Whipple procedure is a complex surgery that involves removing the head of the pancreas, the first part of the small intestine (duodenum), the gallbladder, part of the bile duct, part of the stomach (optional), and nearby lymph nodes. After these parts are removed, we use a portion of the intestine to carefully stitch and connect the remaining parts of the stomach, bile duct, and pancreatic duct using very fine sutures.
For tumors in the body and tail of the pancreas, the surgery is called a distal pancreatectomy. Your surgeon may also need to remove your spleen. If the spleen is to be removed and it’s known in advance, you will need vaccinations. If it is removed during surgery, you will need to be vaccinated around the 15th day post-surgery.
Some people may require the removal of the entire pancreas, a surgery known as a total pancreatectomy. You can live relatively normally without a pancreas, but you will need to take insulin and enzyme medications for the rest of your life.
Surgery for tumors affecting nearby blood vessels: People with advanced pancreatic cancer, where the tumor involves nearby blood vessels, are often not considered candidates for the Whipple procedure or other pancreatic surgeries. However, highly specialized and experienced surgeons may perform pancreatic surgeries that involve removing and reconstructing the affected blood vessels, and they are prepared for such procedures.
After Surgery
Both types of surgeries, whether for the body-tail or the head of the pancreas, are challenging procedures. They are difficult for both the surgeon and the patient. Due to the structure of the pancreas and its location, it is a complex organ to work with. An old surgeon, Theodor Billroth (1829-1894), who introduced many techniques to the world, once said: “God placed the pancreas at the back so that surgeons wouldn’t have to deal with it.” It is clear that it is a difficult organ in terms of location and surgery. Therefore, it must be performed by experienced hands.
When your surgeon discusses the surgical plan with you in detail, they should also inform you about what you may encounter after the surgery. One of these potential complications is bleeding. This can occur during or after the surgery because we are tying off and cutting many vessels during the procedure, and these vessels are quite large and carry a significant amount of blood. There may also be leakage of bile or pancreatic fluid into the abdominal cavity due to suture failure, which can lead to infection or secondary bleeding if previously closed vessels open up. In cases of extensive surgery, patients may sometimes experience diarrhea or difficulty emptying the stomach. One of the most important things I tell my patients is this: We are embarking on a journey together—you, me, and your loved ones—and we will face this situation together. Things may happen, and we must remain strong. Ultimately, there is a possibility of death associated with this surgery. This is a reality, and we will do our best to prevent it.
Chemotherapy and/or Radiotherapy
Chemotherapy uses drugs to help kill cancer cells. These drugs can be injected into a vein or taken orally. You may receive a single chemotherapy drug or a combination of them. Chemotherapy can also be combined with radiation therapy (chemoradiation). Chemoradiation is typically used to treat cancer that has not spread beyond the pancreas to other organs. In specialized medical centers, this combination may be used before surgery to shrink the tumor. Sometimes, it is used after surgery to reduce the risk of pancreatic cancer recurrence.
For individuals with advanced pancreatic cancer and cancer that has spread to other parts of the body, chemotherapy can be used to control cancer growth, relieve symptoms, and extend survival time.
Detailed information about this topic will be provided by an Oncology Specialist when the decision regarding oncology treatment is made.
Can I Seek Help from Alternative Approaches?4o mini
Some integrative and alternative medicine approaches may help with the symptoms you experience due to cancer or cancer treatments.
Treatments to Help You Cope with Depression: People with cancer often experience distress, and this is quite normal. Some studies suggest that distress may be more common in people with pancreatic cancer than in those with other types of cancer. If you are feeling distressed, you may have trouble sleeping and find yourself constantly thinking about your cancer. You may feel angry or sad. Discuss your feelings with your doctor. Specialists can help you sort through your emotions and develop coping strategies. In some cases, medications may be helpful. Integrative medicine and alternative therapies may also assist you in coping with distress. Psychiatric consultations are recommended, but there is also a strong belief in alternative treatments, which you may consider with satisfaction. Examples include:
- Acupuncture
- Art Therapy (engaging in an art form, such as music, painting, etc.)
- Exercise
- Massage Therapy
- Meditation
- Music Listening Therapy
- Relaxation Exercises
- Spirituality (Spiritual Psychology)
If you are interested in these treatment options, be sure to discuss them with your doctor.
Should I Seek Support to Cope?
Learning that you have a life-threatening illness can be devastating. Make sure to learn what you need to know about your cancer. Some family members may try to warn me not to tell the patient about their cancer, saying they will be crushed if I do. However, remember that if you are a family member, they need to be aware of the difficult surgery they will undergo and the treatments that will follow. Being informed about what they will face during and after the surgery can help them navigate this process more easily.
Gather enough information about your cancer to help you make decisions regarding your care. Ask your doctor about the details of your cancer and your treatment options. Request information about reliable sources for more information.
Establish a support system. Ask your friends and family to create a support network for you. They may feel helpless and uncertain after your diagnosis. Helping you with simple tasks can ease their anxiety. And you can relax knowing that you don’t have to worry about specific tasks. Think about the things you might want help with, such as meal preparation or getting to appointments.
Find someone to talk to. Even though your friends and family may be your best allies, they may struggle to cope with the shock of your diagnosis at times. In these situations, talking to a counselor, medical social worker, or pastoral or religious advisor can be helpful. Ask your doctor for a referral.
Connect with other cancer survivors. You may find comfort in talking to other cancer survivors.
Conclusion
When you learn that you have pancreatic cancer, it doesn’t necessarily mean you have to die. With the right treatment and skilled hands, a good surgical outcome can lead to a long life ahead of you. The appropriate surgeon and surgery will inform you about your life expectancy during the post-operative period. While I have patients who have advanced stages post-surgery and pass away within a year, I also have patients who have survived for up to 10 years.

