Gastroscopy
Gastroscopy
General Information
Upper endoscopy is a procedure used to visually examine your upper digestive system with a small camera at the end of a long, flexible tube. A specialist in digestive system diseases (such as gastrointestinal surgery, gastroenterology, or general surgery) uses endoscopy to diagnose conditions affecting the esophagus, stomach, and the beginning of the small intestine (duodenum) and sometimes to treat them.
The medical term for upper endoscopy is esophagogastroduodenoscopy. You can have an upper endoscopy done in your doctor’s office, at an outpatient center, or in a hospital.
Before undergoing obesity surgery, I also want to have a gastroscopy performed myself.
Why is it done?
Upper endoscopy is used to diagnose and, if necessary, treat conditions affecting the upper part of your digestive system, including the esophagus, stomach, and the beginning of the small intestine (duodenum).
To investigate the cause of your complaints: An endoscopy can help your doctor determine the cause of digestive symptoms and signs such as nausea, vomiting, abdominal pain, difficulty swallowing, and gastrointestinal bleeding.
To make a diagnosis: Your doctor may use endoscopy to take tissue samples (biopsies) for testing purposes to investigate diseases such as anemia, bleeding, inflammation, diarrhea, or digestive system cancers.
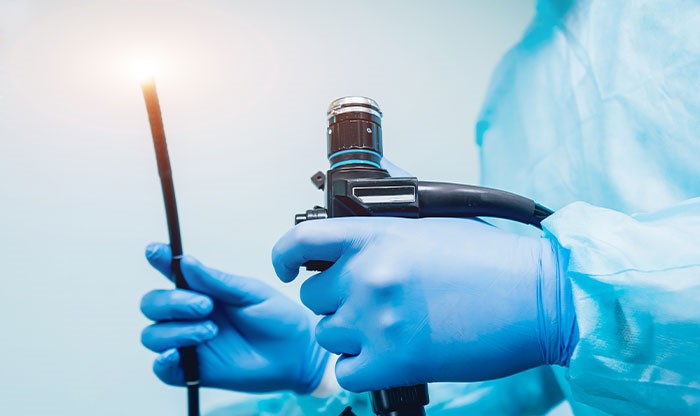
- To treat: Your doctor may use an endoscope to address issues in your digestive system, such as cauterizing a bleeding vessel to stop bleeding, dilating a narrow esophagus, removing polyps, or extracting a foreign object.
An endoscopy may sometimes be combined with other procedures, such as ultrasound. An ultrasound probe can be attached to the endoscope to create special images of the walls of your esophagus or stomach. Endoscopic ultrasound can also help your doctor obtain images of hard-to-reach organs like the pancreas. Newer endoscopes use high-definition video to provide clearer images. Many endoscopes allow your doctor to use a technology called narrow-band imaging, which utilizes special light to better detect precancerous conditions, such as Barrett’s esophagus.
Is it a risky procedure?
Endoscopy is a very safe procedure. Rare complications include:
Bleeding: If the procedure involves removing a tissue sample (biopsy) for testing or treating a digestive system problem, your risk of bleeding complications after the endoscopy increases. In rare cases, such bleeding may require a blood transfusion.
Infection: Most endoscopies consist of examinations and biopsies, and the risk of infection is low. The risk of infection increases when additional procedures are performed as part of your endoscopy. Most infections are minor and can be treated with antibiotics. If your risk of infection is high, your doctor may give you prophylactic antibiotics before the procedure.
Tear (Perforation) of the Gastrointestinal System: A tear in your esophagus or another part of your upper digestive system may require hospitalization and sometimes surgery to repair. The risk of this complication is very low (estimated to occur in about 1 in every 2,500 to 11,000 diagnostic upper endoscopies). The risk increases if additional procedures, such as dilation to widen your esophagus, are performed.
You can reduce your risk of complications by carefully following your doctor’s instructions, such as fasting and stopping certain medications, to prepare for the endoscopy.
When should I suspect a complication?
Symptoms to watch for after your endoscopy:
- Fever
- Chest pain
- Shortness of breath
- Bloody, black, or very dark stools
- Difficulty swallowing
- Severe or persistent abdominal pain
- Vomiting, especially if it is bloody or looks like coffee grounds
If you experience any of these signs or symptoms, contact your doctor immediately or go to the emergency room.
How should I prepare?
Your doctor will provide you with specific instructions for preparing for your endoscopy.
To ensure your stomach is empty for the procedure, you will need to stop eating and drinking four to eight hours before your endoscopy.
Stop taking certain medications: You may need to stop taking some blood-thinning medications a few days before your endoscopy. Blood-thinning medications can increase your risk of bleeding if certain procedures are performed during the endoscopy. If you have chronic conditions like diabetes, heart disease, or high blood pressure, your doctor will provide you with specific instructions regarding your medications.
Be sure to inform your doctor about all medications and supplements you are taking before your endoscopy.
What can I expect?
During the Endoscopy: During an upper endoscopy procedure, you will be asked to lie on your back or side on a table.
While the procedure is in progress: Monitors are typically attached to your body. This allows your healthcare team to monitor your breathing, blood pressure, and heart rate. A sedative will be administered. This medication, given through an intravenous line in your forearm, helps you relax during the endoscopy. Your doctor may spray a local anesthetic in your mouth. This medication will numb your throat as you prepare for the insertion of the long, flexible tube (endoscope). You may be asked to wear a plastic mouth guard to keep your mouth open. The endoscope is then inserted into your mouth. As the instrument passes through your throat, your doctor may ask you to swallow. You might feel some pressure in your throat, but you shouldn’t feel pain. Once the endoscope passes down your throat, you may be able to make sounds, but you cannot talk. The endoscope will not interfere with your ability to breathe.
As your doctor passes the endoscope through your esophagus: A small camera at the tip transmits images to a video monitor in the exam room. Your doctor watches this monitor to look for abnormalities in your upper digestive system. If any abnormalities are found in your digestive system, your doctor may later record images for examination. A small amount of air may be introduced into your esophagus to expand your digestive system. This allows the endoscope to move freely and helps your doctor examine the folds of your digestive system more easily. You may feel pressure or fullness from the added air. Your doctor will pass special surgical instruments through the endoscope to take a tissue sample or remove a polyp. Your doctor will use the video monitor to guide the instruments. When your doctor has finished the examination, the endoscope is gently withdrawn from your mouth. An endoscopy typically takes about 15 to 30 minutes, depending on your condition.
After the Endoscopy: After your endoscopy, you will be taken to a recovery area to sit or lie quietly. You may stay there for about an hour. This allows your healthcare team to monitor you as the sedative starts to wear off.
At home, you may experience some mild discomfort and symptoms after the endoscopy, such as:
- Bloating and gas
- Cramping
- Sore throat
These signs and symptoms will improve over time. If you are concerned or quite uncomfortable, call your doctor.
Do not work for the rest of the day after your endoscopy. You may feel awake after receiving the sedative, but your reaction time will be affected, and your decision-making may be delayed.

